Pinpointing the role of language disruptions in psychosis
By Crystal Mackay, MA’05
Just as a small airport would have challenges handling massive plane traffic, people with psychosis may experience communication difficulties because non-language parts of the brain are trying to manage communications tasks, new research from Robarts Research Institute shows.
Difficulties with communication – the ability to use language and to comprehend what others are saying – are among the earliest symptoms of psychosis, a mental illness characterized by changes in emotions, impaired functioning and a disconnection from reality. Dr. Lena Palaniyappan says the ability of humans to use language may also be what puts us at the unique risk of developing psychosis.
“The language system seems to be key to understanding this illness,” said Dr. Palaniyappan, Professor and Tanna Schulich Chair in Neuroscience and Mental Health at Western’s Schulich School of Medicine & Dentistry and Scientist at Robarts Research Institute and Lawson Health Research Institute. “We don’t yet fully understand how the disorganization of language takes place in patients affected by psychosis.”
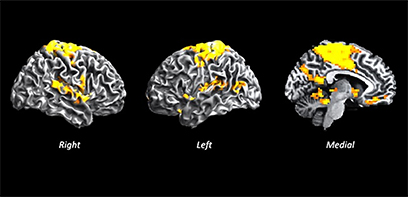
Embarking on a mission to find out, Dr. Palaniyappan worked with a team of imaging scientists at Robarts to perform magnetic resonance imaging (MRI) scans on the brains of patients with acute psychosis. Patients were recruited from the Prevention and Early Intervention Program for Psychoses (PEPP) at London Health Sciences Centre, a flagship clinic that supports young individuals from a very early stage of psychosis.
The team divided the patients into two groups – those with severe language disturbances, and those whose language symptoms were less pronounced. They found that both groups had weakening of connectivity, or ‘hubness,’ in the part of the brain generally associated with language -- the superior temporal area. The group with more severe language symptoms also showed an emergence of greater connectivity in unexpected regions of the brain that seemed to be compensating for some of the loss of connectivity elsewhere.
“This finding led us to believe that the language problems may occur because the main hubs that are supposed to conduct language are now retired, and so these peripheral hubs, which have no business of orchestrating language as their main function, are picking up the job and aren’t doing it very well,” said Dr. Palaniyappan.
The researchers hope that by understanding how language becomes disorganized in psychosis, the data can inform new interventions to focus on strengthening the language systems in the brain to reduce or delay psychotic symptoms.
Using ultra-high-field magnetic resonance imaging at Robarts, they were able to look at the entire brain of patients with acute psychosis. Instead of homing in on one specific area, the team looked at 3-D pixels of the brain (voxels) to get a full picture of what was happening in the whole brain and how different areas were interacting.
Using the airport analogy, Dr. Palaniyappan said that if they had only looked at the language area it would have been like only walking into one airport, and not understanding how the reduced traffic in that airport was influencing the air traffic at other surrounding airports.
“We went in without any expectations, and searched the whole brain,” said Dr. Palaniyappan. “This unique approach allowed us to get a picture of the forest rather than a picture of the tree.”
The study is the first to use this kind of imaging study in patients with acute psychosis who had a wide variety and severity of clinical symptoms.
“Because of the uniqueness of this patient group, we made sure ample time was given to explain the procedure and what was expected," said Joe Gati, PhD, Acting Director of the Western Centre for Functional and Metabolic Mapping at Robarts. "The protocol was kept brief and communication with the subject was maintained throughout the procedure. We also ensured that the imaging protocol was optimized to prioritize data collection, keep noise levels as low as possible, and to minimize the amount of time research subjects were required to be in the MRI.”
The study was funded through an early-career foundation grant from the Canadian Institutes of Health Research and was supported by PEPP.